Peri-implant disease refers to inflammatory conditions affecting the tissues surrounding dental implants. Generally, the literature includes two main types: peri-implant mucositis and peri-implantitis. The importance of peri-implant disease lies in its potential to compromise the stability and longevity of dental implants. If left untreated, peri-implantitis can lead to implant failure, which may require additional surgical interventions and can significantly impact a patient’s oral health and quality of life. Understanding and managing peri-implant diseases are therefore crucial for maintaining the health of dental implants and ensuring their long-term success. Regular monitoring, early diagnosis, and appropriate treatment strategies are essential to prevent the progression of these conditions and to maintain optimal oral health.
But, what is the actual prevalence of peri-implant diseases? That is the topic of This Week in Dental Implants.
New Study: The Prevalence of Peri-implant Diseases is Very High
A new study looked at how common peri-implant diseases are and what factors might be linked to them in people with dental implants. The study concluded 1:
Of the 77 participating individuals, 6 (7.8%) showed peri-implant health, 4 (5.2%) had clinical stability, 35 (45.5%) presented with mucositis, and 32 (41.6%) had peri-implantitis. Among the 343 implants analyzed, 134 (39.1%) had peri-implant health, 13 (3.8%) were clinically stable, 140 (40.8%) had mucositis, and 56 (16.3%) presented with peri-implantitis. Bleeding on probing and the external hexagon platform were significantly associated with mucositis. An increased number of implants per patient, active periodontal disease, and an internal hexagon platform were significantly associated with peri-implantitis. Preventive maintenance did not show a significant association with biological disorders.
These findings suggest that biological peri-implant complications are highly prevalent and may be associated with various patient- and implant-related risk factors, consistent with existing literature. Such characteristics should be considered during early planning stages to help minimize peri-implant biological complications.
Case Photos
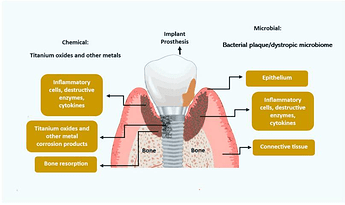
Diagram Showing Potential Etiologies for Peri-implantitis.
Photo Provided By: Ting M, Suzuki JB. Peri-Implantitis. Dent J (Basel). 2024 Aug 9;12(8):251.
Metal corrosion from titanium implants ([Figure 1] may be an initiating factor for inflammation soft-tissue modifications and bone resorption. The mechanisms are not completely understood but may include titanium metal fatigue and stress, reaction to acidic by-products of the bacterial microbiome, chemical reactions to antimicrobial mouth rinses, mechanical damage to debridement by dental practitioners, and chemical reaction to certain diets and alcohol. Further research is required to elucidate these factors. 2
Classification of the Peri-Implant Defects
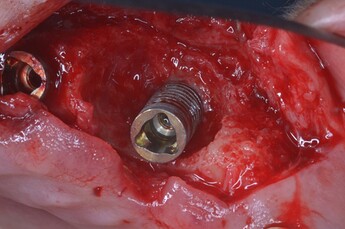
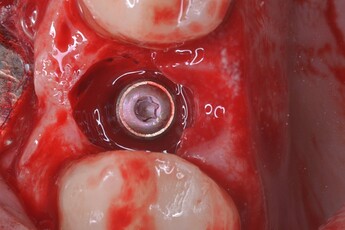
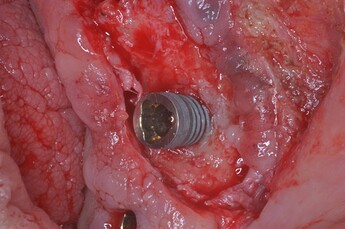
Photos Provided By: Valente NA, Andreana S. Peri-implant disease: what we know and what we need to know. J Periodontal Implant Sci. 2016 Jun
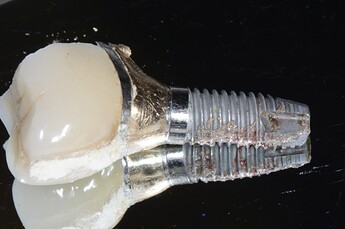
A classification of the peri-implant defect configuration has been proposed by Schwarz et al. (Peri-implant disease: what we know and what we need to know - PMC)] after examining 40 implants affected by peri-implantitis in human subjects and after inducing peri-implantitis in 15 implants placed in five beagle dogs. The defects were classified as Class I when featuring a clear intrabony component (Figure 1and 2), and Class II when the bone resorption was horizontal suprabony (Figure 3). Class I defects were further classified into five sub-categories, according to the configuration of the intrabony component…Current knowledge, although limited, suggests that peri-implant disease is a condition that, while having several traits in common with periodontal disease, is probably much more complex and with unique and distinctive features that need to be thoroughly investigated. A history of periodontitis, lack of maintenance, and cement remnants are certainly factors that play a significant role in the development of the disease and should be addressed from the beginning. (Figure 4 shows an implant removed for advanced peri-implantitis with a clear cement remnant visible on the prosthetic crown.) 3
References
-
Lopes CFFL, Martins BGDS, Motta SHG, Sansone C, Fernandes JCH, Fernandes GVO. Prevalence of Peri-implant Diseases and Association with Risk Factors: A Prospective Cross-Sectional Clinical Study. Int J Oral Maxillofac Implants. 2025 Sep 19;0(0):1-30.
-
Ting M, Suzuki JB. Peri-Implantitis. Dent J (Basel). 2024 Aug 9;12(8):251.
-
Valente NA, Andreana S. Peri-implant disease: what we know and what we need to know. J Periodontal Implant Sci. 2016 Jun;46(3):136-51. doi: 10.5051/jpis.2016.46.3.136. Epub 2016 Jun 29.