This Week in Dental Implants, we review the application of 3D printing for bone graft materials in regenerative dentistry. 3D printing, or additive manufacturing, continues to make rapid advances and has been applied successfully in many various fields, including medicine. The technology also has great potential in dentistry, as evidenced already by the success in various real-world applications like surgical guides, and restorations. (For an excellent overview, see: Application of 3D Printing Technology in Dentistry: A Review. ) But what is the current status of 3D printing as it applies to bone grafting?
3D Grafting: Key Advantage and Current Research
One key advantage of 3D printed grafting materials is that they can be tailored to fit the specific anatomical requirements of patients. This precision in matching the graft to the defect site, can enhance the effectiveness of regeneration. Additionally, 3D printing allows for the incorporation of various biomaterials and growth factors, which can further enhance the biological performance of the grafts. However, despite the promising potential of 3 printing for bone grafts, the few case studies in the literature that we could find (summarized below) are still mostly inconclusive. It is clear that this 3D printing of bone grafts is still at a very early stage, but at the same time, it is certainly an area to watch given the significant advancements in the underlying technology.
Interesting Case Studies
Case Study: Clinical evaluation of 3D printed bone graft for alveolar ridge preservation
The study, Clinical evaluation of 3D printed nano-porous hydroxyapatite bone graft for alveolar ridge preservation: A randomized controlled trial , evaluated the clinical efficacy of 3D printed nano-porous hydroxyapatite in comparison to nano-crystalline bone graft in alveolar ridge preservation prior to implant placement. 1. It concluded that:
Within all parameters of this study, no statistically significant differences were found in alveolar ridge resorption after alveolar ridge preservation with 3DP HA bone graft material or commercial bone graft material (NanoBone®) in terms of 3-dimensional changes of soft tissue and bony tissue, IST value after implantation, and histomorphometric analysis. Overall results indicated that 3DP HA bone graft material can potentially be used as bone grafting material for alveolar ridge preservation.
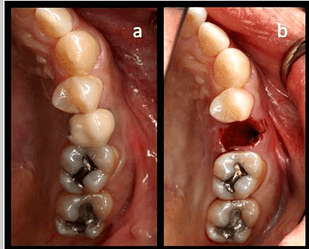
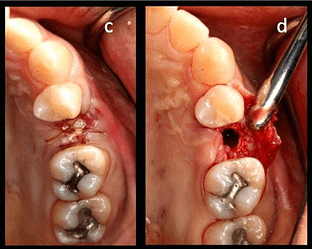
Case photos provided by: Clinical evaluation of 3D printed nano-porous hydroxyapatite bone graft for alveolar ridge preservation: A randomized controlled trial](Clinical evaluation of 3D printed nano-porous hydroxyapatite bone graft for alveolar ridge preservation: A randomized controlled trial - PMC)
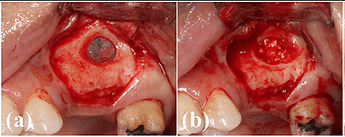
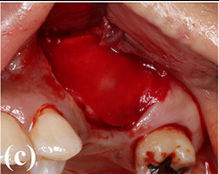
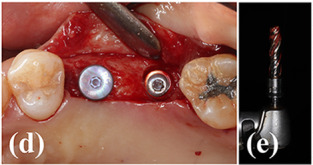
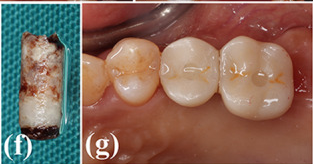
Process diagram of clinical procedure; a) Cracked tooth #25; b) #25 Atraumatic extraction; c) Placement of HA hydroxyapatite granules in alveolar socket after atraumatic extraction, with closing of the socket by Cytoplast™ and suturing; d, e) After four months, harvesting of the grafted area with a trephine bur in formalin solution.
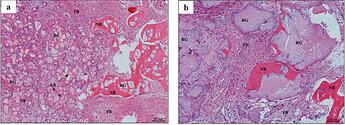
Histological observation four months after surgery. H&E staining demonstrated new bone (NB), fibrous tissue (FB) and residual hydroxyapatite granules (RG) in: a) 3DP HA (test group) and b) NanoBone® (control group) (magnification × 200).
Case Study: Customized 3D Grafts for osseous defects
In the study, Customized three-dimensional printed ceramic bone grafts for osseous defects: a prospective randomized study. , patients were randomly allocated to either a group that received 3D-printed patient-customized bone graft material or a group that received conventional block bone graft material. 2 The study concluded that the 3D grafting materials:
did not demonstrate significant bone regeneration capability compared to conventional graft materials.
Case photos provided by: Customized three-dimensional printed ceramic bone grafts for osseous defects: a prospective randomized study.
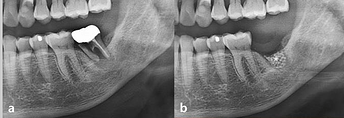
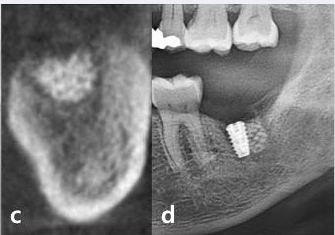
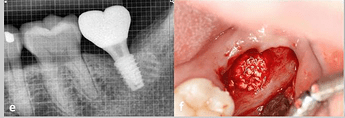
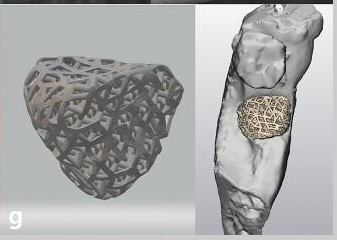
Serial clinical and radiographic images of the experimental group receiving customized 3D-printed ceramic bone grafts. (a ) preoperative panoramic radiograph of tooth #37; (b ) postoperative panoramic radiograph after surgical extraction of tooth #37 with GBR using OSTEON 3D and Collagen Membrane; white asterisk indicates grafted bone material; (c ) CBCT image before the implant placement at visit 5; (d ) panoramic radiograph after implant fixture installation; (e ) panoramic radiograph after final implant final prosthesis; (f ) clinical photo of bone grafting; (g ) 3D digital image of design for fabrication of customized 3D printed ceramic bone grafts (OSTEON 3D).
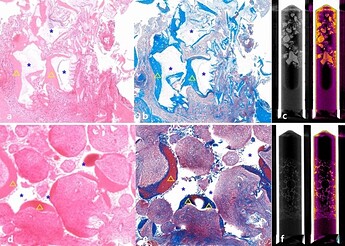
Histological and radiological examination. (a ) Hematoxylin and eosin (H&E) staining of harvested bone from the experimental group; (b ) Masson’s trichrome staining of harvested bone from the experimental group; (c ) Micro-CT examination of harvested bone specimen in the experimental group; (d ) H&E staining of harvested bone from the control group; (e ) Masson’s trichrome staining of harvested bone from the control group; blue asterisk indicates grafted bone material; yellow triangle indicates newly formed bone; (f ) Micro-CT examination of harvested bone specimen in the control group
.
Case Study: 3D Printed Graft for Sinus Augmentation
In the study, Polycaprolactone Impregnated 3D Printed Nanohydroxyapatite for Sinus Augmentation: A Randomized Controlled Trial, the researchers compare the effect of polycaprolactone impregnated 3D printed nano‐hydroxyapatite (3DPHA‐PCL) with bovine bone substitute material (BB) in lateral maxillary sinus floor elevation. 3 They concluded that:
Dimensional stability of the augmented bone was comparable between the groups. However, group 3DPHA‐PCL demonstrated inferior new bone formation and implant survival compared to group BB. Long‐term follow‐up is warranted to monitor the behavior of 3DPHA‐PCL.
Case photos provided by: Polycaprolactone Impregnated 3D Printed Nanohydroxyapatite for Sinus Augmentation: A Randomized Controlled Trial
Characteristics of 3DPHA‐PCL. (a) Clinical view of 3DPHA‐PCL particles. (b, c) Scanning electron microscopic images of the particle.
Clinical photographs of the surgery. (a) A bony access window was created on the lateral wall of the maxillary sinus. (b) 3DPHA‐PCL was filled in the sinus after detaching the sinus membrane. (c) A collagen membrane was applied to cover the access window. (d) Dental implants were placed on #15 and #16 areas. (e) A bone core biopsy was performed during drilling. (f) The obtained specimen. (g) An implant prosthesis was delivered (#17 was extracted).
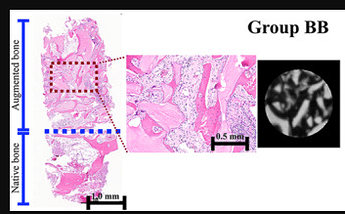
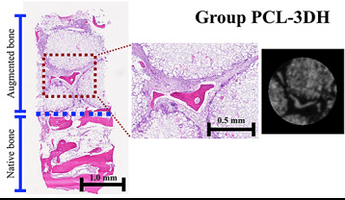
Representative histological and micro‐CT images of groups BB and 3DPHA‐PCL. Group BB, lateral MSFE using bovine bone substitute material; Group 3DPHA‐PCL, lateral MSFE using polycaprolactone impregnated 3D printed nanohydroxyapatite.
References
-
Kijartorn P, Wongpairojpanich J, Thammarakcharoen F, Suwanprateeb J, Buranawat B. Clinical evaluation of 3D printed nano-porous hydroxyapatite bone graft for alveolar ridge preservation: A randomized controlled trial. J Dent Sci. 2022 Jan;17(1):194-203.
-
Kim NH, Yang BE, On SW, Kwon IJ, Ahn KM, Lee JH, Byun SH. Customized three-dimensional printed ceramic bone grafts for osseous defects: a prospective randomized study. Sci Rep. 2024 Feb 10;14(1):3397.
-
Thammanoonkul P, Limpattamapanee S, Thammarakcharoen F, Suwanprateeb J, Lim HC, Buranawat B. Polycaprolactone Impregnated 3D Printed Nanohydroxyapatite for Sinus Augmentation: A Randomized Controlled Trial. Clin Exp Dent Res. 2025 Oct;11(5):e70237.
-
Chen Y, Wei J. Application of 3D Printing Technology in Dentistry: A Review. Polymers (Basel). 2025 Mar 26;17(7):886. doi: 10.3390/polym17070886.